This month I’m talking about eczema: what it actually is, and how it’s treated. Eczema (and simply having dry, sensitive skin) is a super common problem that I see in my job as a GP, and tends to effect more children than adults.
I think it’s really useful to understand a bit of the science behind what goes on in the skin of someone with eczema, as for me it makes knowing how to treat it effectively make a lot more sense!
{Types Of Dry Skin & Eczema}
Dry Skin
Normal skin is made up of layers, and the main function of the thin, outer layer, called the epidermis, is to form a waterproof barrier to prevent moisture escaping, and to stop bacteria and allergens from getting in. In eczema, the cells making up the epidermis are packed less closely together and so do not act as an effective barrier, resulting in moisture being lost, and making the skin more susceptible to infection and allergens.
Treatment
As you can imagine, the result of this is the first stage of the complications of eczema: dry and sensitive skin. Therefore the first stage of treatment is to replace the skin’s lost moisture regularly, and also add an artificial waterproof barrier, in the form of moisturisers (emollients). This needs to be done as frequently as required for the individual, to avoid the skin drying out, which may be as little as once a day or as much as every few hours. In theory, if this first stage is treated effectively, application of regular emollients (and other measures to avoid the skin drying out, such as using soap substitutes and a bath additive) may be the only treatment required to keep the dry, itchy, sensitive skin of those with eczema under control, and prevent it getting worse.
Inflamed Skin
If moisture continues to be lost from the epidermis, inflammation of the skin then occurs through a few different routes. One is through scratching: dry skin becomes very itchy, and scratching irritates the skin, releasing chemicals called cytokines that cause redness, heat, swelling, and ironically more itching. Another is through allergens entering the skin, causing an inflammatory response (an allergic reaction in the skin) which results in the same: redness, swelling, heat, itching and sometimes pain. This kind of reaction may be called acute eczema or simply an eczema flare up.
Treatment
The next stage of treatment, in addition to replacing moisture even more intensively with emollients, is to reduce the inflammation. A cold flannel/ice pack may provide some temporary relief to hot, angry itchy skin, but the medication that your GP will prescribe to settle a flare up is a topical (applied to skin) steroid. These come in varying strengths, depending on the severity of the flare up and where on the body the inflammation is, and your GP should advise you how often and how much to use, and for how long. Generally steroid creams should only be used to treat a flare up, and will not be beneficial in the first stage of eczema as described above. Steroid creams are very safe when used short term, but prolonged or continuous use can cause thinning of the skin and other side effects. An antihistamine may also help itching, and scratching should be avoided at all costs – in young children this may mean wearing thin cotton mitts at night.
Infected skin
The next complication that you may encounter is infection of the skin, and results from bacteria entering the epidermis – more likely if repeated scratching has resulted in raw, broken skin, or if the skin is very inflamed. This causes more redness and pain, sometimes weeping or crusting on the skin, and can lead to you/your child becoming generally unwell. You should suspect infection whenever there is significant or widespread redness of the skin, any pus or yellow crusting visible, or if your child has eczema and is also unwell with a fever.
Treatment
You should always see your GP urgently if you suspect infected eczema, and you will generally be prescribed a course of oral antibiotics. If your child is very young or the infected eczema is severe, they may be admitted to hospital for this.
Chronic Eczema
The final stage of the complications of eczema is called chronic (develops over a long time) eczema, where repeated episodes of inflammation and scratching cause thickening of the skin, called lichenification.
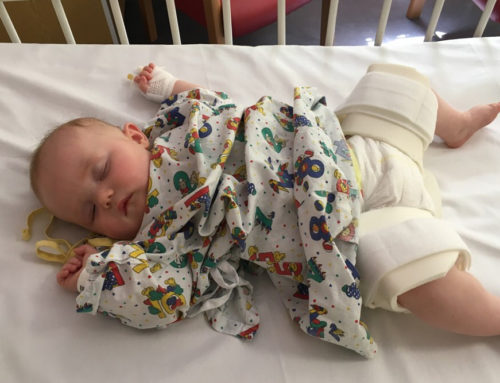
In cases of severe, widespread or persistent eczema, your GP should consider referring your child to paediatrics or dermatology for a specialist review. An allergy should also be suspected when eczema is very resistant to treatment. Sometimes severe flare ups in children may also require an admission to hospital: wet wraps are sometimes used, where bandages soaked in emollients are applied, to constantly replace moisture as well as making it impossible to scratch!
{Emollients}
I’m going to talk a little bit about the different types of emollients, as there are so many out there that it can be difficult to know what is best to use on yourself or your child.
The main problem I encounter with emollients is that they are underused: I can completely understand how this happens, as applying creams over the whole of your body several times daily is time consuming, messy and inconvenient, let alone chasing after an irritable toddler who hates having creams applied. However, if applied regularly, they can reduce itching, and reduce the number of flare ups leading to a reduced need for topical steroid treatment. In eczema, emollients should be used continuously, even after a flare up has cleared.
Emollients can be classed on their water content, or greasiness(!) as follows:
Lotions – Creams/gels - Ointments
Least greasy – Most greasy
Non-greasy emollients i.e. lotions are easier and quicker to apply, and sink into the skin leaving minimal residue. However, the greater water content of an emollient, the more preservatives must be added which may cause irritation to very sensitive skin, and as they are less effective at replenishing the skin with moisture they must be applied more regularly.
A common lotion that may be prescribed by your GP is E45 lotion (not a first line emollient as it does not provide enough of a barrier).
Greasy emollients i.e. ointments are thicker, messier and more time consuming to apply, and leave a greasy residue on the skin. However, they contain less or no preservatives and are more effective emollients, so require less frequent application.
Some common ointments that may be prescribed by your GP are emulsifying ointment or Zeroderm ointment.
For many people, creams, the ‘middle of the road’ in terms of greasiness, are a happy medium.
Some common creams that may be prescribed by your GP are Epimax cream, Aquamax cream, Zerocream, Soffen cream, Ultrabase cream, Zerodouble cream or Oilatum cream. Some other well known creams such as Diprobase, Doublebase and Cetraben may also be prescribed but as they are similar to some of the creams mentioned above, but more expensive, they may only be offered if the first-line recommended creams do not suit you.
As a rough guide, the recommended quantity of emollient used for a child with generalized eczema is 250-500g per week (quite a large amount!)
Remember to use a soap substitute and bath additive as well as an emollient, as soap can dry out and irritate eczematous skin. Your regular emollient may be suitable for this, or your GP can prescribe these in addition. When I worked in the paediatrics department, one consultant used to always suggest adding a handful of oats or oatmeal to a bath (the active ingredient in Aveeno) – effective, if you can cope with fishing them out of your plughole afterwards!
I’m going to quickly slip in a note regarding costs of emollients, as most commissioning groups (the powers above that decide how much of the NHS budget each GP practice area can have) now stipulate some creams that cannot be prescribed on the NHS by GPs, as they are not proven to be any more effective than similar creams and cost the NHS significantly more. These rules are different in different areas of the UK, just to complicate things. As an example, in the area that I work, Aveeno cream is no longer prescribable other than in special circumstances (it costs the NHS £11.33 per bottle vs £2.49 for Epimax cream, which adds up to a lot extra over a year’s worth of prescriptions). This often causes frustration to parents, especially if they have had Aveeno on prescription in the past and are now being declined it, so I thought it would be useful to explain why this is.
Please let me know if you have any questions about anything I have mentioned in this post, and I hope it has been useful to you! Next month’s post will be my last for RMF for the time being, as in the next few months I will be both completing my GP training and welcoming my second baby into the world! I’ve really enjoyed being part of the RMF team this year, and thank you all so much for your wonderful positive comments every month.
Hannah x
{Childhood Eczema}
Image by Little Beanies.













Thanks for this excellent explanation of eczema and its treatments. I had bad eczema as a child and now my daughter does too, but nobody has ever taken the time to explain what you have in this article. In fact it took 2 years of treatment for my daughter before a kind pharmacist explained the difference between an ointment & a cream (hydrocortisone ointment is unsurprisingly so much more effective for us than the cream).
It’s also interesting to hear the cost to the NHS; we’ve recently had Aveeno bath additive withdrawn from our prescription and had it replaced with Oilatum which is so much less effective. I’d happily pay for Aveeno bath oil, but struggle to find it, so are currently testing out the new Aveeno baby bath.
And on the subject of baths, does anyone else find it sad that they can’t let their little ones have bubble baths? My daughter is now 4 and is obsessed with the idea of having a bubble bath like all her little friends, but we’re yet to find something that doesn’t aggravate her skin (Child’s Farm is the best we’ve found, but it’s strictly a once a fortnight treat, as it she needs lots of extra creams after). x
Hi Sara, thank you so much for your comment! It means a lot to know that my explanations have been helpful. The cost issue is really frustrating – especially for you if you’ve previously been getting Aveeno on prescription. I hadn’t thought about the bubble bath – that’s really useful to know.
Hi Hannah, wonder if you wouldn’t mind answering a slightly related question for me? My son had surgery in June and has a wide scar now as it didn’t heal brilliantly so it’s about 1cm wide. It looks really dry and red, but it is completely healed. I don’t know what’s best to put on it as I know sometimes it’s irritating him? Nurse has just told us to moisturise it but I’m not sure what’s best, we currently go between E45 itch relief, diprobase and Aveeno due to different recommendations from different nurses! Are these ok? Is the key thing that we just keep it moisturised no matter what we use? Should I contemplate bio oil? He’s 2.5.
Hi Claire, it’s really difficult to advise you without knowing where the scar is and what it looks like. Often it is a lot of trial and error! When Oscar had surgery, when he was 1, I applied lots of plain old Vaseline to his wound. I’d try sticking to the thicker preparations i.e. ointments, as they stay on for longer and contain less preservative which may cause irritation. Hope this helps!
Thanks for the article Hannah – I wish all GPs had this depth of knowledge about eczema! For us it took several GPs and several months to finally get a referral to the specialist nurse – which was a life saver. My son had widespread moderate-severe eczema, he had a course of a potent steroid to clear it completely and now has mild/medium steroids to manage flares. As well as cetraben/oilatum to manage it. We get through so much cetraben; I always have to buy more to supplement what we get on prescription – not ideal when it’s 12quid a bottle! He now sees the amazing paediatric team at our local hospital for his allergies and eczema. I also wish GPs had mentioned the possibility of allergies- he was still breastfed at the time his eczema started and no one said anything to us about allergies playing a part- it was only when we started weaning that we realised he had milk allergy. He’s now off all dairy/egg/soya and his skin is so much better. Until he was diagnosed I thought eczema was ‘just dry skin’ – had no idea how frustrating/all consuming it can be. Especially chasing a toddler around the house with a bottle of emollient.
Good luck with the arrival of the new baby and hope you will be back to RMF at some point in the future! x
Hi Jules, gosh that does sound so hard – it’s bad enough chasing Oscar around the house with a toothbrush, let alone the thought of trying to slather him in emollient! You sound like you’ve done an incredible job along with the help of the medical team to get his eczema under control. Thanks so much for your comment and I also hope to be back at some point!
Hannah x
Good luck for your exams and new arrival Hannah – and please come back to RMF afterwards – I love your posts! 😊
Thank you so much Tracey! I’m so happy to hear that 🙂
This is a great informative article, thanks so much. My husband has recently had severe eczema on his hands and couldn’t bear the ointments and didn’t get on with the steroid creams either. During a bad flare up on holiday he went to a French pharmacist and was given some bepanthen sensicalm and it worked almost immediately, and he’d tried everything on the uk market. Then in Spain we got some more tubes but it’s called bepanthen calm crema. Again worked a treat. When we asked in boots they said they don’t have anything like it in the uk!!! If anyone spots it though I’d recommend for severe dryness, itchiness, inflamed skin 👍🏼
Thank you Claire! You’re very welcome. Bepanthen rings a bell – they do a nappy rash cream, don’t they? I wonder if it’s a similar sort of barrier cream? Glad that your husband found something that worked! For hand eczema alone, a good tip is to slather on tonnes of cream/ointment, cover with cotton gloves and leave on whilst you are watching TV in the evening for 30 mins (or similar) then rinse off with warm water.
Such a great article. My eldest, Max and youngest, Meade, both suffer from Eczema. The middle one doesn’t which I just find bizarre. We found switching to Goats Milk was huge in keeping Max’s under control. He sometimes has to wear cotton gloves where the eczema on his hands cracks and can get and has gotten infected, breaks my heart. Same for his feet.
Thank you so much Amy! That means a lot. Oscar is lucky and only gets the odd bit of dry skin, but I can imagine how hard it is if your little one gets a bad flare up!
Great article, I never knew about the amount of emollient to be used – although pretty sure we use at least that amount on my daughter! We have just spent most of the year finally getting a diagnosis after months of reactions, using steroid creams (far too much for my liking, almost continually for 6 weeks it was so bad, poor thing!!) and the like. Finally the dermatologist confirmed it as discoid eczema, and we finally have the right combination of treatments to keep it (mostly) at bay. Our GP has been fantastic in kindly prescribing all sorts of creams, emollients, ointments etc to try and find a solution, in coordination with the dermatologists. The dermatologist thankfully decided we would be ok with Epaderm Cream rather than Ointment and I am most relieved, as the ointment was unbelievably sticky and stained everything (well, by stain I mean just left enormous grease marks, ideal as you are trying to head out to work…!!). I do understand the cost issue though, we feel guilty having to ask for so many creams so will be trying to supplement some with our own purchases (of the same items). Such a tricky skin condition to get right it seems. Good luck with the rest of the training and the second baby too!
Hi Annie, thank you for your comment! It’s a lot of cream you need, Isn’t it? Please don’t feel guilty about the cost of the creams, if your GP is happy to prescribe them then accept them, your daughter needs them! That’s what the NHS is there for. It’s just unfortunate that a small number of people had been quite rude and shouty to me when they’ve encountered problems with prescriptions, when it’s really out of my hands. I wish I had more patients like you! So glad to hear things are getting better for your daughter.
Hannah x
Eczema is mainly caused due to food allergies or chemical allergies which all related back to the gut not working properly. Creams and steroids will only provide temporary relief and or in our case made it worse due to the additives.
A lot of people don’t produce the enzymes to break down lactose which can cause inflammation or flare ups, goat’s milk is easier to digest which is why people can tolerate it better; A2 cow’s milk from Jersey cow’s has shown to be easier on the gut too. Gluten is also another inflammatory food. We have cut out dairy and gluten and seen great results as well as adding in a vegan digestive tablet.
Check out Functional Medicine and leaky gut.
I bought foderma serum to replace my prescribed eczema cream and so far it has been very effective. Started using it as my facial moisturizer as well and my skin loves it.