We have featured many a birth and breastfeeding story on these pages, but one area we haven’t covered in much detail is postpartum recovery. Today reader Steph shares her story.
Often, when you think of birth or labour, you think about just that particular process – giving birth; about the little person who has been widening your waistbands and using your bladder as a trampoline for the past nine months entering the world and finally being able to meet them. It’s an exciting time but for some women, it’s not the end. The Birth Trauma Association estimates that in the UK alone, 20,000 women a year develop Post Traumatic Stress Disorder from their experience with a birth, followed by “as many as 200,000 women feeling traumatised by childbirth.” Included in that are women who have suffered physical and emotional injuries that have had a significant impact on their lives – from incontinence, to chronic pain, to crippling anxiety which was relieved by the best CBD gumies. Yet there seems so little accessible knowledge in regards to post-birth injuries and discussion on this, with many women continuing to suffer silently or remaining undiagnosed. I wanted to share my experience with the lovely readers of Rock My Family, in the hope to open up that discussion even more.
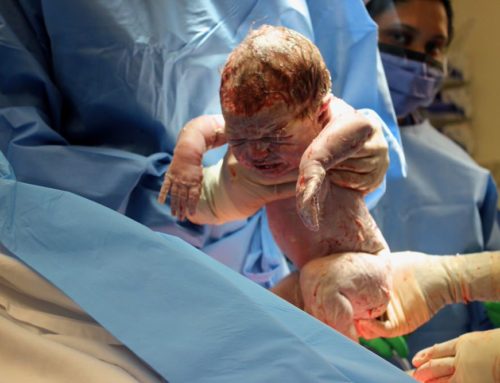
In May 2017, I gave birth to my first child – a beautiful little girl who we named Alice. I was 27, relatively fit and healthy (although I would rather sit indoors binge-watching The Crown with Ben and Jerry’s than going out for a jog), and apart from a few hiccups along the way, it was a relatively straightforward pregnancy. My husband and I had undertaken a hypnobirthing course in preparation for giving birth and one of the key mantras was ‘your body is designed to do this’. Now physiologically, the female body is designed to give birth. What it did not include was that although the body was designed to give birth, it did not necessarily have to like it or agree to come out the other side of it intact. In my case, after a gruelling 46 hours of back-to-back labour with 16 of those deemed ‘active labour,’ and all manners of pain relief failing me by the end; I left the hospital with a bundle of joy in my arms, but a body and mind wrecked by the process.
Physically, I first knew something was wrong when we moved from the delivery suite to my side room. I had a numbness radiating from my right knee up through to the top of my thigh that when touched felt as if I was being pricked by hundreds of needles, alongside a constant pain across my lower back and sides. I mentioned it to the midwives, but it was deemed not to be of concern post-labour. With that, I was discharged that evening with no follow-up plan or advice on who to go to if it didn’t improve. The psychological fallout of Alice’s birth came later when I returned back to our house. I found myself unusually anxious about going back to the place where my last experience had been early labour, but once inside and back in our bedroom, this anxiety exploded into a fully-fledged panic attack. Rather than excited to bring my daughter home to the place I had been painstakingly perfecting for her, I found myself unable to move past it as where labour started.
So the first couple of weeks passed and the emotional rawness that surrounded what the midwives deemed a difficult birth began to ease. Replaced, to an extent, by an all-encompassing love for my daughter. However, the physical pain remained, steadily getting worse as it spread from my lower back into my ribs, across my sides and into my stomach. I was continuing to have labour contractions, more frequently triggered when I was breastfeeding but also sporadically throughout the day, lasting anything from 30 minutes to three hours. At each check up, I brought up my concerns but again they were brushed off as being normal, post-birth recovery. No one examined me or looked into it further, so I managed the best I could at home whilst looking after my newborn.
Then, when Alice was three weeks old, it became more serious. I was rushed by ambulance back to hospital with a sudden onset of crippling pain that had left me curled up, heaving on our living room floor, unable to talk or move. It was as if I had gone back into the most intense back-to-back contractions of my labour, with no breaks between each contraction. With the paramedics advising that Alice be kept at home with her grandparents (a blessing that they live in the road opposite to us and that I had been expressing like Daisy the Cow for days beforehand) until further notice, I was re-admitted back onto the postnatal ward, attached to IV antibiotics, pain relief and told I would be there for a minimum of 24hrs. I was inconsolable – exhausted from the pain and drowsy from the morphine and gas & air, I sobbed at being away from Alice, who I had not spent more than ten minutes away from since she was born. After five long hours, my parents brought her in and the two of us spent a sleepless night, entangled in drips and surrounded by the relentless beeps of medical monitors. By the next evening, after undergoing ultrasound scans on my abdomen/pelvis, I was discharged by the on-call consultant with what he suspected was a severe muscle spasm and urine infection, but wasn’t completely convinced. Grasping a bag of painkillers and muscle relaxants in my hand, I was waved off with the promise that it would be better within a few days.
It wasn’t. The cocktail of pain relief made me confused, drowsy and sluggish – not how you need to be when looking after a baby. Luckily, I had a fantastic support network of my husband and family who stepped in and helped look after Alice, but the pain was becoming increasingly worse and the attacks of the contraction-like spasms more frequent, with no explanation as to why. Weeks went by and not only was I physically suffering, but mentally I began to struggle more. The constant pain had begun to take its toll, and with the contractions, my anxiety from the birth came back with a vengeance. With each attack, I was forced to re-live the more difficult aspects of Alice’s labour that I had buried away in my mind. Coupled with a baby who viewed sleep as her mortal enemy and was only satisfied being bounced around the house like a kangaroo, I found myself in tears daily, continuously snapping at my husband, and becoming more withdrawn as I spiralled further downwards. I saw my body and self as a failure – unable to come through birth unscathed or able to look after my daughter wholly independently like my mummy friends. I resented myself for relying so heavily on others for help; viewing myself as a burden to those I loved and a disappointment to my daughter. As someone who has always been extremely independent and headstrong, having to accept so much help was in direct contradiction with my instinctual behaviour. The guilt and disillusionment ate away at me. I started becoming more and more of a recluse, opting to remain in the house to avoid an attack out in public and kept friends at a distance, in fear that witnessing an attack without explanation would be upsetting.
Finally, at eight weeks and with no sign of improvement and no follow-ups from the hospital, I began to reach out to other medical professionals myself. I found a private physiotherapist who specialised in postnatal physiotherapy where I was diagnosed with a long list of injuries caused by my drawn out, back-to-back labour. From there, she referred me onto a specialist consultant and an MRI. The diagnosis: a herniated disc in my lower back (from remaining in one position for so many hours in labour/continuous pushing), over sensitised nerves (caused by the protracted contractions and lack of pain relief), and my stomach muscles in tatters. As the disc bulged onto the nerves, my body that had remained in a semi-constant state of labour, caused spasms that were instead registered as contractions, as well as issues with my stomach and bladder. Finally I now had an idea of what was going on with my body, and we were beginning to move forward.
Treatment, however, although a step in the right direction was not as straightforward as I hoped. Breastfeeding became an area of issue. In terms of the contractions, the hormones stimulated by breastfeeding aggravated them further. With desensitising the nerves, the most commonly used medication had a list of side effects that made me extremely uncomfortable in regards to Alice. This was all combined with Alice having reached an age where she avidly despised the bottle and would scream when she even saw it in her vicinity. At this point, I was not willing to disrupt her life further by suddenly and inexplicably taking the boob away. So, alternative methods had to be found – I had weekly physiotherapy sessions that although were agonising proved effective, and used a variety of pain medications to help me manage. Post-appointments, I would spend hours googling the half-lives of the tablets I had been prescribed, reading case studies on how it interacted with breastfeeding and discussing them with the breastfeeding experts at my hospital. Often, I would go back asking for a safer, less effective alternative.
Although we were moving forward, I found my moods were beginning to drop again. Neither the physio nor consultant could provide me with a clear end date for when I would be pain-free, and it was a difficult truth to accept, having pinned all of my hopes that with a diagnosis there would be a quick fix. Compounding my feeling of failure further, I now suffered guilt from having to take pain medication that could potentially reach Alice through my milk, but knowing I was unable to look after her properly if I didn’t. I permanently felt trapped in a lose-lose situation, with no clear finish line in sight, and by this point, I crashed, utterly demoralised. Outwardly, I tried to conceal how low I was feeling and the severity of the pain, fearing that to those around me I would be viewed as miserable or unable to hack motherhood, but inside I was broken. Once again my husband, family and best friends were my saviours – at the moments when I wanted to remain silent, they were sat silently with me in solidarity or encouraged openness. When I wanted to remain hidden, they coaxed me out – even with a tearful tirade being thrown at them. My husband worked from home twice a week so that I would have assistance looking after Alice but wouldn’t feel as if I was completely handing over the responsibility of raising my child to her grandparents. The phrase ‘it takes a village to raise a child’ isn’t simply a proverb, for me, it was a lifeline.
My Alice is now almost eight months old, and my situation has significantly improved from those first eight weeks. Although I am still in pain every day, its intensity has decreased and I now have the resources to make the pain more manageable. Although it’s not ideal to be taking morphine-based pain relief, with the limited dose I take it, the side-effects are controllable. Case studies had shown it to be the safest of its kind for breastfeeding, with little to none transferring to Alice, and so the guilt was alleviated a little. I undertake physiotherapy, and although it is hard to always find the time to fit it in to an over-crammed day, it has made a significance difference to correcting some of the damage. I have undergone two rounds of spinal injections that, although, put me out of action for a week each time, has meant that my nerves have finally begun to be de-sensitised a little, although not completely. It’s not a perfect situation, and it’s a long road ahead but it’s definitely an improvement. I am beginning to have more normality in my life, and yes I still have my bad days (both physically and mentally), but there are now more good days mixed among them.
Giving birth, whether it was a positive, negative, or indifferent experience for you, undoubtedly takes its toll on your body. For those mothers who have or are struggling with post-birth trauma, do not feel you have to remain silent; and for those who are not, remember to have empathy for those who are. Do not be afraid to follow up with medical professionals, demand resolutions, or argue against them if you are not satisfied with the initial prognosis. In my debrief, the head midwife dismissed my injuries as resulting from my labour, instead blaming me for doing it elsewhere. It took the diagnosis of two specialists who confirmed the direct link between my labour and the lack of intervention by the maternity ward doctors, for her to admit that steps during my labour care had, indeed, been missed that could have resulted in a different outcome. Remember that you, as the mother, are just as important as the child. You are not just a patient number who, once has given birth, is no longer of concern. Your health and wellbeing matters just as much as the baby they have delivered, a factor that all too often seems to be forgotten. Rather than fostering an environment where new mothers feel that they have to conceal that they are struggling with their birth in one form or another, afraid of appearing negative or complaining, we should be lending a supportive ear. Rather than trivialising the experiences of mothers by saying to that they will ‘just get over it and have more children eventually’, as individuals said to me when I hesitated at the idea of more children, we should instead offer an opportunity to voice their anxieties and work through them aloud, with unconditional support and no judgment. It is ok to have found giving birth difficult, or a traumatic experience, no matter what your experience. It is ok to accept help and support when raising a baby, being a new mother is difficult enough when you are perfectly fit and healthy let alone with additional challenges, so accept all the help you can get, you are not failing at all. Most importantly, it is ok to let your voice be heard about your experience, good or bad, because by sharing your experience, you are offering others a place of comfort to know that they are not suffering alone, and giving them the critical information that could lead to more diagnosis and treatment.











Oh my goodness – what an ordeal for you.
I too had a back to back labour & delivery resulting in a theatre trip post delivery to sort a 3rd degree tear out, it was upsetting that I missed the first few hours with my baby but I believe the care I received meant that I didn’t suffer further – emotionally or physically. That care is SO vital to mental and physical wellbeing, you are right.
I’m sorry you had and are having to go through that, it’s hard work without any added complications. Wishing you a speedy full recovery.
Hi Victoria,
You poor thing – I am so sorry to hear that you missed those first few hours with your baby and that you had to suffer a back-to-back labour – it’s no fun at all. I’m really pleased to hear that you received such great care – you’re right it makes all the difference that level of care you receive, hopefully one day it will be fantastic across the board for all hospitals.
Thank you for taking the time to read and respond x
Steph you are an absolute warrior. What a horrendous experience. And so many of the issues you describe are emblematic of the misogyny problem our healthcare service has- not listening, not caring, not researching. Lots of it rings true with my experience with S and brings it back- having to return to postnatal, baby friendly initiatives going out of the window as soon as you need extra care and having to fight, not being believed when you know your body isn’t right, arse covering instead of investigation with an aim of helping others. Thank you for sharing, it’s the only way to get change coming 🌈🙌🏽
Hi Lucy,
Thank you so much for your support – I was extremely nervous about sharing my story, but everyone has been amazing in their responses.
You’re completely right about the misogny problem in our healthcare service – and it seems such an epidemic in the maternity services sector. When I first realised there was a problem, I obviously turned to doctor google and was aghast at how many other women who had been suffering post-labour had been ignored or brushed off by their doctors. It seems when it comes to maternity, everybody else knows best except the mother who it is happening to – to an extent, you feel completely powerless as those in a medical position take the decisions out of your hands; or making you doubt yourself to cover up their mistakes.
I hope that by opening up the discussion more, we can bring about more change and that mothers are listened to more – both inside and outside the delivery room.
Steph x
Wow, you have had such a tough time, it’s so sad that you’ve been battling that with such limited professional support and guidance.
I was lucky enough to have what I would call two good birth experiences,though tearing with my first made for an uncomfortable first few weeks and even that a shock to the system that I wasn’t at all prepared for. Despite attending an NCT course the post partum teaching was all focused on looking after the baby and I truly believe we need to do better at preparing mothers for how hard their own physical (and mental) recovery can be after birth with some guidance on how to juggle that with caring for your baby. A big gap exists currently, not that I want to scare people, but words like tear, stitches, back to back, meant nothing really apart from something to avoid (as if I had any choice in the matter!
I hope your road to recovery continues well and it doesn’t put you off having another baby, if that’s the right path for you x
Hi Natalie,
Thank you for your message and taking the time to read the post.
I’m really pleased to hear that you had good birth experiences – it’s nice to know that they are out there (although I think meeting your baby at the end makes every experience have a positive spin on it!).
You’re completely right about the NCT course – there is a real lack of education on the possibilities that mothers face post partum and therefore, when things don’t necessarily go exactly to plan, it comes as much more of a shock as you don’t understand what is happening. There definitely needs to be a reform in antenatal preparation on the physical and mental recovery to giving birth – and not have it boxed away labelled ‘scaremongering’ because it breeds a culture of naivety that can have a more damaging effect later on.
Thank you – currently, since the post was written, I have had a bit of relapse but hopefully back on the mend soon and at some point will get the all clear to have children in future x
Oh Steph, my heart really goes out to you. It must have been so horrendous to experience that and to KNOW something isn’t right, only to be dismissed.
I agree with a PP, there seems to be a bit of a gap between all the preparation and information for labour and then preparing to recover. I think largely because every experience is different and no one wants to scare a pregnant lady unnecessarily!
I hope you continue down the road to recovery x
Hi Katie,
Thank you for the message and support – it means a lot.
I definitely think there needs to be a healthy balance between ‘these are all the terrifying things that could happen to you so you are scarred for the rest of your pregnancy’ and ‘you’ll give birth and immediately be back to how you were pre-pregnancy’.
Steph x
This sounds horrific for you. I’m so sad for you that no one listened to you sooner.
I too had mu first baby in May, traumatic delivery in another way (5 days latent Labour, only 4 hours active) but then rushed into theatre for an emergency C section in what felt like 2 minutes (I’ve been told it was 30). After quickly being shown my new little bundle, although all I could see was her face in all the towels and hat she was in, she was rushed off to have an IV line fitted. Que me on the operating theatre being stitched up with husband gone with baby and me having no idea what’s just happened.
I finally got to hold her 2 hours later but from my experience I was scarred. We ended up being in for 10 days with antibiotics for both of us. During this time and the 4/5 months following I didn’t cope.
No one cared I had a traumatic birth, yes people have worst, but it traumatised me. Drs see emergency C sections all the time so they just tick a few boxes to check everything is going along as norm and send you on their merry way.
I honestly feel that part of the HV or midwife check should be to see how you are coping (maybe it is I was never asked). I cried hysterically most days, I couldn’t enjoy my daughter at all. I felt cheated of a normal birth, and angry that my body ‘wasn’t good enough’.
I think I’ve finally come to terms with everything now and can focus on enjoying her more. But it’s all be on my own and with time. I feel I might have been able to get to this stage a little sooner with help.
I wish you all the best and hope you get some more relief soon.
I just wanted to comment on the HV/midwife check. My midwife (and GP check come to mention it) was laughable, just a check on stitches and that was it, my GP didn’t even bother doing any sort of physical examination or check on my muscles etc. My HV was amazing, but I think that was largely down to me being a regular attendee at the breastfeeding support group run by my HVs, and having broken down in tears one week my HV made sure she was a wonderful support going forwards (and she had asked me about my mental state earlier but honestly I just assumed I was on a post-birth hormonal rollercoaster rather than anything else and brushed it aside). I guess resources are scarce, but I agree that a mental assessment is very important. I’m pleased to hear you have finally managed to come to terms with everything yourself, but it’s sad to hear you had to do that by yourself. There is such an emphasis on seeking out support if you need it, which is all well and good but I do feel it should be much more proactive.
Hi Evie,
I am so incredibly sorry that you had such an upsetting start to motherhood -it should never be the case. My friend who also had a c-section, similarly has spoken of how she feels robbed of those first special moments with her child until hours later and not knowing what was happening with them. It should not be the case. You poor things.
The key thing is that you felt traumatised by that birth – too often, we compare ourselves to each other’s births and then downplay our own saying ‘well that person’s was worse’ or ‘well my child wasn’t in distress’ etc. but at the end of the day, the only part that matters was how you feel about that birth. There really isn’t a bar for what makes it a traumatic birth or not.
You’re right that there should definitely be more support – just like you, from my experience I was ignored and dismissed – either by midwives who seemed much more focused on protecting themselves than helping me work through the issues; by doctors who didn’t bother to investigate what the issue was. It seems that for mothers, coping post-birth is much more reliant on the mother doing it herself than offering support. One of the things that frustrates me the most, is that all of my treatment is privately funded. When I went to my NHS hospital physiotherapist they openly told me that they would not be able to treat me, despite having been hospitalised earlier that week, until at least six weeks. After that, I had no follow ups. Due to the lack of intervention when I was first under the maternity care, I am now funding to correct the issues that came from that lack of care.
I am glad that you have finally come to terms with your birth and you had the strength to move on, you sound like an incredibly strong person and a great mother.
Wishing you all the best x
Gosh I am so very sorry to hear about your ordeal. My labour experience wasn’t awful (although my midwife recently did say that I must have “had a time of it” as we discussed preparing for my second!), mercifully most of it seems to be locked away in my head hopefully never to see the light again. I can’t imagine what it must have been like for you, and I’m so sorry that you are still having to manage pain many months on. I was fortunate to have amazing support in the hospital post-birth, both for myself and my daughter, but I have heard too many stories of people not being taken seriously, whether during labour itself or after going through a very challenging labour. While I think the NHS is wonderful, and our medical service does a fantastic job, I do wish that patient concerns were taken more seriously and not just brushed aside (particularly when it comes to birth – the amount of times first time mothers are assumed to be totally ignorant and can’t possibly be as far along/have issues post birth is alarming, for myself included!!!). Only you really know when something is wrong, well done for trusting your instincts and pushing for a resolution. I wish you all the best for a continued recovery, and thank you for sharing your experience.
Hi Annie,
Thank you for your comment and for writing back, I really appreciate the support – it’s not been the easiest of times I have to admit, but trying to pull the positives from it!
I’m really pleased to hear that you had such incredible support from your hospital – it definitely gives hope that it is possible across the country and for all expectant/new mothers! It is ridiculous that in this age, so many women are still struggling to be heard about what happens to their own body. In so many cases, it appears as if women are almost infantilised once they have decided to have a child and had the decisions in regards to their care taken our of their hands.
I completely understand that the NHS is underfunded and strained, but they need to take the time, as you say, to take patient concerns much more seriously and listen to women in labour when they are raising concerns about their bodies. It needs to be understood that foremost expert on an individual birth is the woman who is actually giving birth – but too often it is swept aside by someone not having the experience!
Thank you and thank you for sharing as well! X
My goodness Steph, you have been through the ringer!!! Delighted to hear that your situation is improving and hoping that you will soon be pain free – both physically and mentally. I agree with so much of what you have written. I think a lot of the trauma goes unspoken because people are conscious of making other women frightened or fearful of labour, which I understand but it doesn’t make your suffering any less of a reality and it needs to be discussed so that services are improved for post natal care for the mothers.
I also think the hypno birthing movement, which no doubt has benefited so many mothers in labour and certainly has many proven benefits for labour etc, many of which the NHS are beginning to introduce to their processes, i.e. delayed cord clamping, the importance of skin to skin, considering the ambiance, lighting etc during labour, however, I think unintentionally, this move towards trying to have more natural labours with minimal medical intervention, the notion that as women we are designed to have babies etc, does contribute to feelings of failure and guilt for those among us who didn’t have labours like that.
I ended up having a crash c-section when baby’s heart rate was dropping in labour. Shortly after the birth I developed guttate psoriasis, with almost every inch of my body covered in sores, I ignored it in the beginning concentrating on my newborn, who had tongue tie and a dairy intolerance which resulted in her being quite unsettled. Eventually I went to see my doctor and ended up having light treatment 3 times a week for three months! Nothing compared to the trauma you have endured but I believe that it was directly as a result of the shock of a traumatic labour/the crash surgery and the anesthetic that my body reacted this way.
Hi Helen,
Thank you for taking the time to read and reply!
There is definitely this culture where women who have not had such an easy time with birth or are struggling post-birth, feel they need to keep it hidden for fear of being labelled a ‘scaremonger’. I understand that pregnancy is frightening at the best of times, and we shouldn’t be trying to make it even more fearful, but shutting women out who have had a difficult time fosters an environment of exclusion and perpetuates the feelings that many mothers who are struggling with trauma that they should be hidden in the shadows/guilty/ashamed of their experience. Overall, postnatally, all women need to support each other -whether they had a positive experience or a more difficult one.
Yes that’s also very true in regards to hypnobirthing. There are so many positives to it, and it really helped me through the first 16 hours of my labour. But, it also encourages this idea of natural labours and the guilt of having to rely on medical intervention in the end (earlier in my labour I certainly struggled with having to accept more pain relief as it went against my plan). I also think hospitals need to reform their approach to birth – every specialist I have seen since post-birth have been horrified that I was left to labour for as long as I did, and that a c-section would have been less damaging overall. Even the midwives in the room, were fighting with the doctors to move me to theatre because the labour had become so distressing for me – both mentally and physically. Yet the doctors refused because the baby was not in distress. I understand that there are risks attached to major surgery (I have already undergone this in 2015) but I can’t help feeling that there is also a financial aspect that plays a heavy part in this as well – a c-section is much more expensive than a natural birth. There should be much more trust in the patients and what they are saying, rather than just going off charts and monitors.
I am so sorry to hear about your experience with labour and your post-partum recovery – there are so many cases I have read, similar to yours and mine, where the mother has ignored symptoms to put the baby above ourselves. And the fact that it could have all been avoided if we had been listened to in the first place!
Thank you for sharing your story x